Are you struggline with skin picking? Treatment for Dermotillomania can help
Skin picking (aka Excoriation Disorder) is a behavior that is not known or understood by most doctors. Needless to say, implementing a cookie-cutter approach in skin picking treatment will yield little or no improvement in the people treated by nonexperts. Each person has a different motivation behind their picking and treatment needs to help people who engage in this body-focused repetitive behavior to take control over their urges.

What are the symptoms of Dermotillomania?
Excoriation (Skin Picking) Disorder Excoriation disorder, also known as skin picking disorder, is characterized by repetitive manipulation of the skin causing tissue damage. According to the Diagnostic and Statistical Manual of Mental Disorders (5th Edition) of the American Psychiatric Association, excoriation disorder is defined as meeting the following criteria:
- Recurrent picking at the skin resulting in skin lesions.
- The skin picking is not better explained by symptoms of another mental disorder (e.g., delusions or tactile hallucinations in a psychotic disorder, attempts to improve a perceived defect or flaw in appearance in body-dysmorphic disorder, stereotypes in stereotypic movement disorder, or intention to harm oneself in non-suicidal self-injury).
- Individuals must have made repeated attempts to decrease or stop the excoriation.
- The skin picking causes clinically significant distress or impairment in social, occupation, or other important areas of functioning.
- The skin picking is not attributable to the psychological effects of a substance (e.g., cocaine) or another medical condition (e.g., scabies
*The International Statistical Classification of Diseases and Related Health Problems “ICD-10) contains codes for trichotillomania and skin picking disorder. We favor the criteria and description used in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5).
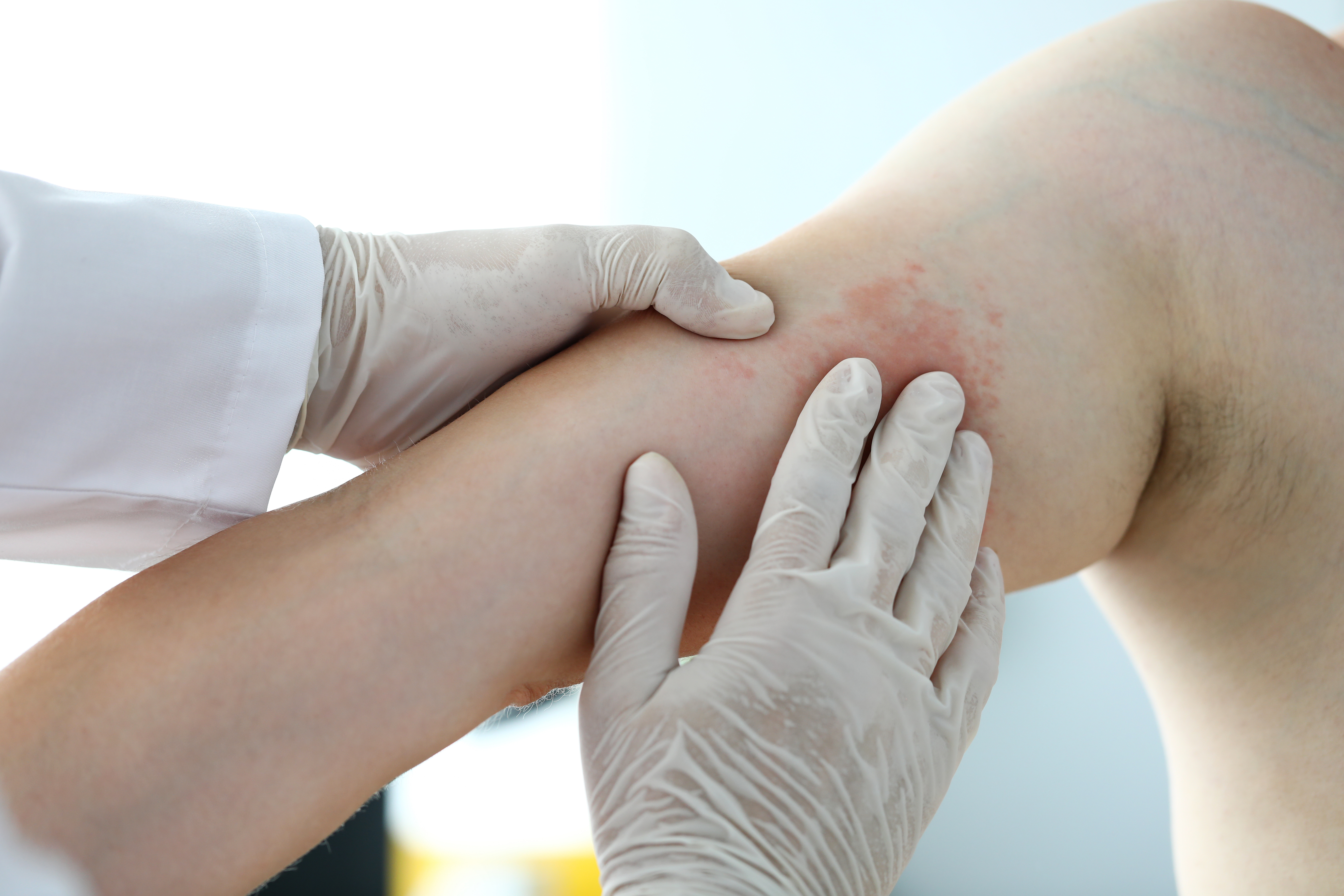
What does Treatment for Dermotillomania look like?
The most important thing that a person can do to address a BFRB is first to become knowledgeable about the problem and its treatment. A psychotherapy approach called cognitive behavior therapy (CBT) is the treatment of choice for BFRBs. Existing studies suggest that CBT is superior to medication in treatment outcomes.
However, some individuals may need medication first or in conjunction with CBT if there is an underlying or comorbid psychiatric diagnosis (i.e., depression, anxiety, ADHD) that may be triggering more urges to pull.
Cognitive Behavior Therapy CBT is a therapeutic approach that focuses on identifying thoughts, feelings, and behaviors that are problematic and teaches individuals how to change these elements to lead to reduced stress and more productive functioning. An emphasis is placed on matching the treatment to the unique symptoms of the individual.
There are a number of different treatment approaches for BFRBs that fall under the umbrella of CBT: habit reversal training (HRT) and comprehensive behavioral treatment (ComB).
Acceptance and commitment therapy (ACT) and dialectical behavior therapy (DBT) are two treatment approaches that may bolster the effectiveness of other cognitive behavior therapies.
Habit Reversal Training Habit reversal training (HRT) is an early treatment for BFRBs developed in the 1970s by Nathan Azrin and Gregory Nunn.

What is HRT for Dermotillomania?
HRT is the method that has been examined most in research studies. HRT has a varying number of components in its treatment package. The three components that are considered most critical are awareness training, competing response training, and social support.
Awareness Training
Awareness training consists of helping the person focus on the circumstances during which pulling is most likely to occur. This enables individuals to become more aware of the likelihood that the behavior will occur, and therefore provides opportunities for employing therapeutic techniques designed to discourage performance of problem behaviors.
Competing Response Training
Competing response training teaches the individual to substitute another response for the pulling behavior that is incompatible with the BFRB. For example, when an individual experiences an urge to pull, he/she would ball up their hands into fists and tighten their arm muscles and “lock” their arms so as to make pulling or picking impossible at that moment. This response is to be repeated each time that individual experiences an urge to pull or pick or when faced with a situation where pulling or picking is likely to occur.
Social Support
Social support involves bringing loved ones and family members into the therapy process in order to provide positive feedback when the individual engages in competing responses. They may also cue the person to employ these strategies and provide encouragement and reminders when the individual is in a trigger situation.
The research literature encourages using HRT for short-term improvement; however, professionals and sufferers have found that when used by itself, achieving long-term improvement in symptoms is much more difficult. Whether we are setting personal goals of losing weight, changing eating habits, smoking cessation, or committing to exercise 4x a week, we as humans all perform MUCH better when we have a coach, trainer, friend, romantic partner, or therapist to be accountable to.
Working with an expert in the area of TTM treatment increases your success rate dramatically. Dr. Ori has been in practice for over two decades and has successfully treated thousands of Trichotillomania sufferers.
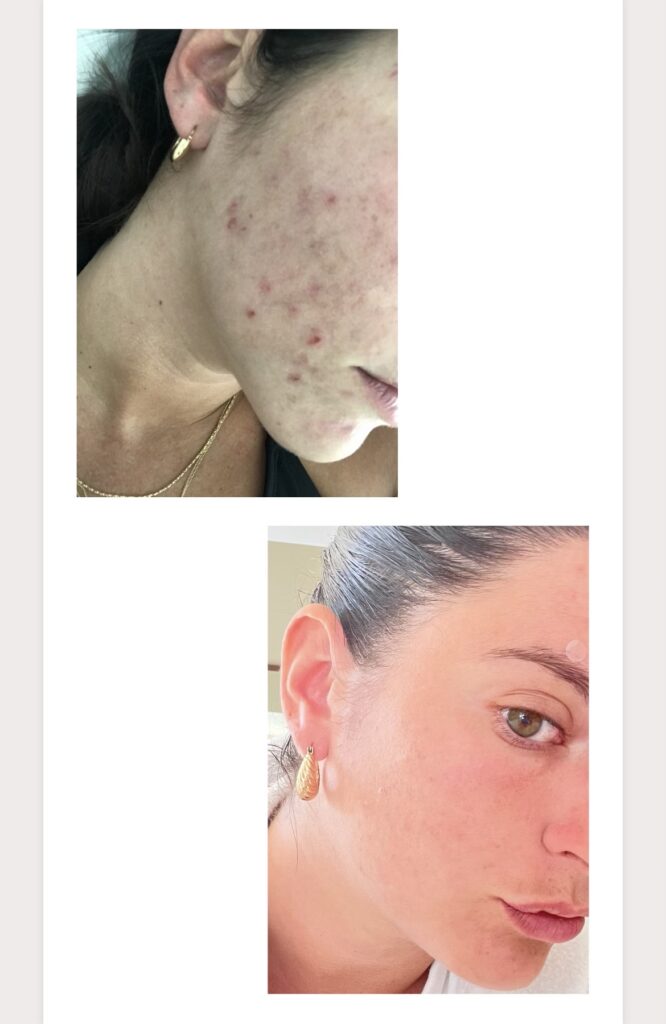
** photo permission granted by the client
What is the goal of Demotillomania treatment?
The goal of weekly treatment is to reduce your skin-picking behaviors and replace them with healthier alternatives. With those who are highly motivated, significant improvements can be seen within the first couple of months of treatment.
Most clients will reduce picking behaviors by 50% in the first month and up to 75% in the second month of treatment. Clients typically find that the final handful of “picks” per week is the most stubborn, but once they reach zero “picks” for 5-6 consecutive weeks, we can reduce treatment frequency from weekly to biweekly sessions.
Skin picking treatment switches over to “relapse prevention” to help reduce the likelihood of relapse. If the client continues to be “pick-free,” we reduce to monthly “booster” sessions until we both decide it is time to terminate treatment.
Several clients decide at this point to continue weekly sessions to work on reaching other personal/psychological goals, i.e. anxiety reduction, ADD-related executive function skills, and strategies, depression reduction, social anxiety treatment, career goals, and/or relationship issues.
Getting Started is Easy!
You can contact Dr. Ori Shinar via email, phone, or by scheduling a free 15-Min Consultation.
After meeting with him, you will be explained about the logistics of therapy, including his availability, insurance reimbursement, in-person versus online therapy, and finally scheduling your initial (60 minutes) consultation session.
Afterward, weekly (45 minutes) sessions will continue until you meet your therapy goals.
